Request Appointment
Our Location
Monday
Closed
Tuesday
8:00 am - 5:00 pm
Wednesday
8:00 am - 5:00 pm
Thursday
8:00 am - 5:00 pm
Friday
8:00 am - 1:00 pm
Saturday
Closed

Wisdom teeth, medically known as third molars, are the final set of permanent teeth to develop. For many people they appear in late adolescence or early adulthood, but their timing and position vary widely from person to person. While some individuals have enough space for these teeth to erupt comfortably, others experience alignment problems, incomplete eruption, or teeth that remain trapped under gum tissue or bone.
Because wisdom teeth erupt so late, they can interact with a fully developed dental arch in ways that earlier teeth do not. Crowding, pressure on adjacent molars, and food trapping behind partially erupted teeth are common issues. Even teeth that appear symptom-free at first can create subtle changes over time—such as gradual shifting of neighboring teeth or pockets of tissue prone to inflammation.
Recognizing the role third molars play in oral health is the first step toward making an informed decision about care. Our goal in explaining these basics is to help patients understand why some wisdom teeth can be safely monitored while others require surgical attention.
An impacted tooth is one that cannot fully erupt into its expected position. Impacted wisdom teeth may be covered by gum tissue (soft tissue impaction), by bone (bony impaction), or by a combination of both. Each scenario presents different risks: soft tissue impactions can create flap-like pockets that trap bacteria, and bony impactions may exert pressure on adjacent roots or lead to cyst formation over time.
When wisdom teeth cause trouble, the symptoms can range from intermittent discomfort to acute infection. Pain, swelling, difficulty opening the mouth, recurrent gum inflammation around the back teeth, and persistent bad breath are signs that merit evaluation. In some cases, impacted third molars contribute to decay on neighboring teeth or even begin to affect the health of the jawbone.
Not every impacted tooth will lead to immediate problems, but leaving high-risk wisdom teeth in place can increase the likelihood of future complications. That’s why careful assessment—based on symptoms, clinical exam findings, and imaging—is important to determine the most appropriate plan for each patient.
A thorough evaluation typically begins with a focused history and clinical examination. Your clinician will ask about symptoms such as pain, swelling, or recurrent infections and will examine the mouth for signs of inflammation, pockets of trapped food, and the position of the third molars relative to surrounding teeth. This hands-on assessment helps identify immediate concerns and guides the need for further imaging.
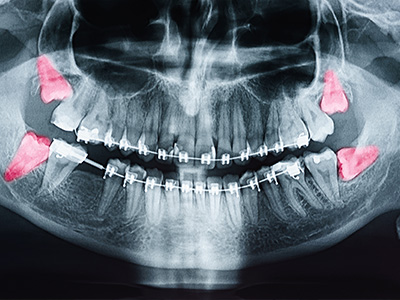
Radiographic imaging is often a key part of the assessment. Panoramic X-rays or cone-beam CT scans provide a detailed view of tooth position, root structure, and relationships to critical anatomy such as the inferior alveolar nerve and the sinus floor. Imaging helps classify the type of impaction and predict surgical complexity, which informs both the treatment recommendation and the discussion about risks and benefits.
When appropriate, we’ll explain the findings in plain language and outline options—ranging from active monitoring to removal—tailored to your age, symptoms, and overall dental plan. Our priority is to ensure you understand the rationale behind each recommendation and to answer any questions you have before moving forward.
Wisdom tooth removal is a common oral surgery performed under a variety of anesthesia options to maximize comfort. Depending on the complexity of the case and patient preference, procedures can be done with local anesthesia, nitrous oxide, IV sedation, or general anesthesia. The goal is to create a calm, pain-free experience while maintaining patient safety throughout the procedure.
Surgical technique varies according to the tooth’s position and surrounding anatomy. Simple extractions involve removing a fully erupted tooth with minimal manipulation, while impacted or bony extractions may require a small bone window or sectioning of the tooth to allow safe removal. Meticulous technique and careful handling of soft tissues help minimize postoperative swelling and promote predictable healing.
Our team places emphasis on intraoperative communication and postoperative instructions that support a smooth recovery. Before the procedure begins, we review what to expect during and immediately after surgery, including anesthesia effects, temporary dietary restrictions, and basic measures to reduce bleeding and swelling. Clear preparation helps reduce anxiety and improves outcomes.
Healing after wisdom tooth extraction typically progresses over several days to a few weeks. During the first 48–72 hours, some swelling, mild discomfort, and minor bleeding are common. Following the instructions provided by your surgical team—such as rest, cold compresses, and appropriate oral hygiene adjustments—can make the early recovery phase more comfortable and lower the risk of complications.
As the site heals, gentle rinsing, avoidance of strenuous activity, and a soft diet help protect the surgical area. Long-term healing of bone and soft tissues continues for weeks, and routine follow-up ensures that the site is progressing as expected. It’s important to report any unusual signs—such as severe, persistent pain unrelieved by medication, increasing swelling after several days, persistent fever, or continuous bleeding—so that your clinician can evaluate and manage those concerns promptly.
For many patients, timely removal of problematic third molars prevents recurring infections and protects adjacent teeth. Whether you’re experiencing symptoms now or are monitoring developing wisdom teeth, an individualized assessment will determine the safest and most appropriate path forward. If you’d like to learn more about your options, contact us to discuss your situation and schedule an evaluation.
Wisdom teeth are a normal part of dental development for many people, but their late arrival and variable positions mean they sometimes pose challenges. Early, careful assessment helps differentiate teeth that can be observed from those that benefit from removal. When extraction is recommended, modern surgical techniques and anesthesia options focus on safety, comfort, and predictable healing.
If you have questions about your third molars or are experiencing symptoms that concern you, reach out to our office to arrange an evaluation. Our team at Pharos Implants and Oral Surgery is available to review your case, explain the options clearly, and help you make the best decision for your oral health.

Wisdom teeth, also called third molars, are the last permanent teeth to form and usually appear in late adolescence or early adulthood. Their timing and position vary widely, so some people experience eruption without issues while others encounter crowding or partial eruption. Because they emerge after the rest of the dental arch is established, wisdom teeth can interact with neighboring teeth in ways earlier teeth do not.
Not everyone develops all four third molars, and some people lack them entirely. When wisdom teeth are properly aligned and fully erupted they may function normally, but unpredictable positioning makes careful evaluation important. A thoughtful assessment helps determine whether observation or removal is the safer option for long-term oral health.
Pain and complications often arise when a wisdom tooth cannot fully erupt or is misaligned. Partially erupted teeth can create flap-like pockets that trap food and bacteria, leading to recurrent gum inflammation, bad breath, or localized infection. Pressure from an erupting third molar can also contribute to crowding or cause decay on adjacent teeth when hygiene is difficult to maintain.
In addition to soft-tissue issues, wisdom teeth that are impacted against bone or adjacent roots may create areas of chronic irritation or lead to cyst formation over time. Symptoms can range from intermittent discomfort to acute infection with swelling and difficulty opening the mouth. Early detection and monitoring reduce the chance of more significant problems developing.
Impaction describes a tooth that cannot fully erupt into its expected position, and third molars are commonly classified by how they are blocked. Soft tissue impaction means gum tissue covers part of the tooth, while bony impaction indicates the tooth is encased in or blocked by bone; many cases involve a combination of both. The type of impaction influences symptomatic risk and the technical approach needed for safe removal.
Soft tissue impactions often create pockets prone to infection, while bony impactions can place pressure on adjacent tooth roots or be near anatomical structures such as the inferior alveolar nerve. Recognizing the impaction type helps the surgeon predict complexity, discuss potential risks, and plan the most appropriate surgical technique. Proper imaging is essential to make this distinction clearly.
Evaluation begins with a focused medical and dental history and a clinical examination to assess symptoms, mouth opening, and signs of inflammation or trapped food. Imaging is a central component; panoramic radiographs provide an overall view of tooth position while cone-beam CT scans offer detailed three-dimensional information about root anatomy and proximity to nerves and the sinus floor. These findings, combined with age and overall dental needs, guide whether to monitor or recommend extraction.
During the consultation the clinician will explain findings in plain language, classify the impaction, and outline the likely course if teeth are left in place versus removed. The assessment also identifies any factors that affect surgical risk, such as medical history or medication use. Clear communication ensures you understand the rationale for a recommended plan and what to expect next.
Several anesthesia options exist to maximize comfort and safety during wisdom tooth removal, and the choice depends on case complexity and patient preference. Local anesthesia numbs the area for simpler extractions, while nitrous oxide offers mild sedation and anxiolysis for nervous patients. For more complex or multiple extractions, intravenous sedation or general anesthesia can provide deeper sedation and complete comfort during the procedure.
Your surgeon and care team will review medical history and explain the benefits and considerations of each option before recommending an approach. Safe monitoring and experienced anesthesia techniques help ensure a calm, pain-free experience. Postoperative instructions will vary slightly depending on the anesthesia used, so understanding those differences is important for recovery planning.
Surgical technique is tailored to the tooth’s position and surrounding anatomy; a simple, fully erupted tooth may be removed with minimal manipulation, while impacted teeth often require more involved steps. For bony impactions the surgeon may create a small bone window, section the tooth into pieces, and carefully remove fragments to minimize trauma to adjacent structures. Throughout the procedure the focus is on precise technique and gentle tissue handling to reduce postoperative swelling and promote predictable healing.
Hemostasis and suturing are performed as needed, and the team reviews immediate postoperative expectations before discharge. Clear intraoperative communication helps patients remain informed and comfortable throughout care. The surgeon will also discuss follow-up appointments to monitor healing and address any questions that arise after the procedure.
Initial recovery commonly involves some swelling, mild to moderate discomfort, and minor bleeding for the first 48–72 hours. Following postoperative instructions—such as rest during the first day, use of cold compresses, and taking prescribed or recommended medications—can significantly improve comfort and reduce the chance of complications. Maintaining gentle oral hygiene and avoiding vigorous rinsing or straws helps protect the surgical site in the early stages of healing.
Most routine activities can resume over several days, but complete bone and soft-tissue healing continues for weeks. If pain increases after the first few days, bleeding persists, or you develop a fever, contact the surgical team promptly for evaluation. Regular follow-up ensures the site is healing as expected and addresses any concerns in a timely manner.
While most extractions heal without major issues, potential complications include infection, dry socket, prolonged bleeding, and temporary nerve disturbance. Dry socket, a painful disruption of the normal clotting process, typically appears three to five days after surgery and is managed by the clinician with gentle irrigation, medicated dressings, and pain control. Infections are treated with drainage if necessary and appropriate antibiotics based on clinical findings.
Nerve injuries are uncommon but can cause altered sensation to the lower lip, chin, or tongue when the inferior alveolar or lingual nerve is involved; most nerve changes are temporary and monitored closely. Your surgeon will review the specific risks identified on imaging and the measures taken to minimize them, and will provide clear guidance for prompt evaluation and treatment if complications arise.
Decisions about proactive removal are individualized and depend on factors such as the patient’s age, symptoms, tooth position, and likelihood of future problems. Younger patients often heal more quickly and may benefit from removal if imaging predicts impaction that could damage adjacent teeth or lead to recurrent infections. Conversely, fully erupted, symptom-free third molars in patients with excellent oral hygiene may be appropriate for periodic monitoring rather than immediate extraction.
Surgeons weigh the current condition against the probability of future complications when making recommendations, and they discuss the expected benefits and risks of either approach. Regular dental checkups and updated imaging help ensure timely intervention if a previously monitored tooth begins to pose risks. A personalized plan provides the best balance between preserving teeth and preventing avoidable problems.
To arrange an evaluation, contact the office to request an appointment or to speak with a member of the care team about your concerns and symptoms. During the visit Dr. Joshua Munson or a member of the clinical team will take a medical and dental history, perform a focused examination, and obtain imaging as needed to form a clear treatment recommendation. The consultation is designed to answer questions about risks, anesthesia options, and the expected recovery process so you can make an informed decision.
Our Cornelius office will help coordinate scheduling and provide any pre-appointment instructions, including guidance about medications and arrival times. If you are experiencing acute pain, swelling, or signs of infection, inform the staff when you call so they can prioritize urgent evaluations. Clear communication before and after your visit helps ensure safe, efficient care tailored to your needs.

Our friendly and knowledgeable team is ready to help you schedule appointments, answer questions about procedures, and address any concerns. Whether by phone or our easy online contact form, we’re here to make your experience simple and convenient.
Take the first step toward restoring your smile and discover the difference personalized, expert care can make. Contact us today and let us help you achieve the confident, healthy smile you deserve.