Request Appointment
Our Location
Monday
Closed
Tuesday
8:00 am - 5:00 pm
Wednesday
8:00 am - 5:00 pm
Thursday
8:00 am - 5:00 pm
Friday
8:00 am - 1:00 pm
Saturday
Closed
Sedation dentistry helps patients undergo oral surgery with less fear and more comfort. For many people, the idea of a surgical procedure triggers anxiety that can make visits difficult or avoidable. Sedation provides a controlled way to reduce that stress, allowing patients to remain calm — or even sleep through the treatment — while the surgical team manages pain and safety.
When delivered by a trained oral and maxillofacial surgeon, sedation is part of a comprehensive plan that balances comfort, medical history, and the specific needs of the procedure. At Pharos Implants and Oral Surgery, our approach emphasizes clear communication and careful monitoring so each patient receives the level of sedation that is appropriate for their situation.
Sedation dentistry addresses two common barriers to care: anxiety and sensitivity to pain. By reducing nervousness and minimizing awareness of the procedure, sedation allows patients to remain relaxed and cooperative. This can shorten appointment times and improve the overall experience, especially for complex or multiple procedures performed in a single visit.
Beyond comfort, sedation can improve procedural precision. A relaxed patient is less likely to move unexpectedly, which helps the surgeon work more efficiently and safely. Many patients also report less post-operative distress because their memory of the perioperative period is diminished or absent.
Safety is central to the use of sedation. Oral and maxillofacial surgeons receive specialized training in anesthesia and airway management, and sedation is always delivered in an environment equipped for monitoring and emergency response. Local anesthetic remains a routine part of every procedure so that the surgical site is numb even when sedation is used.
Deciding which sedation method to use starts with a thorough preoperative assessment. This includes reviewing your medical history, current medications, past anesthesia experiences, and any conditions that may affect breathing or cardiac function. This information helps the surgeon determine the safest and most effective option for each patient.
We also evaluate the nature of the procedure: some treatments require deeper sedation for patient comfort and procedural efficiency, while others can be completed comfortably with lighter methods. The team explains the expected effects, recovery timeline, and any necessary day-of instructions so patients can make an informed choice.
Consent and communication are essential. Before moving forward, patients receive clear guidance about what to expect during and after sedation, including safety precautions such as arranging a responsible escort when deeper sedation is planned. Our goal is to create a tailored plan that prioritizes safety and minimizes anxiety.
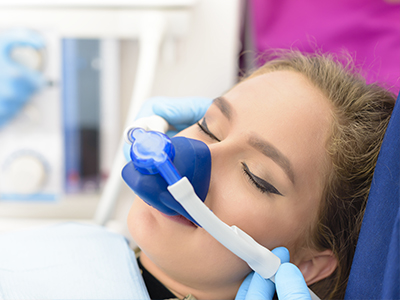
Nitrous oxide, often called “laughing gas,” is a mild inhaled sedative that produces relaxation without eliminating consciousness. Administered through a small nasal mask, it takes effect rapidly and can be adjusted throughout the appointment. Because its effects wear off quickly once the gas is stopped, recovery is typically swift.
This option is well suited for patients who feel nervous but want to remain awake and communicative during treatment. Nitrous oxide is easy to combine with local anesthetic, and it carries a low risk profile when used by trained clinicians. After treatment most patients feel clear-headed and can resume normal activities shortly after their appointment, though individual instructions from the surgical team should be followed.
While nitrous oxide is effective for many, it may not provide enough sedation for more invasive procedures or for people with severe dental phobia. During the preoperative evaluation the team will indicate whether nitrous oxide is a suitable choice or whether a deeper option should be considered.
Oral sedation involves taking a prescribed medication before the appointment to produce a state of calm that ranges from mild drowsiness to more pronounced relaxation. The medication is typically taken at a recommended time before the procedure so it reaches an effective level during treatment.
Oral sedatives are a practical option for patients seeking a predictable, less intrusive form of sedation. Although patients remain responsive, many experience reduced memory of the procedure and a strong sense of relaxation. Because the effects vary from person to person, the surgical team provides specific preoperative guidance and recovery expectations.
Patients using oral sedation must follow the practice’s safety instructions, which include having a responsible adult accompany them to and from the appointment. The surgeon will also review any medications or medical conditions that could interact with oral sedatives to ensure a safe experience.
Intravenous (IV) sedation delivers sedative medications directly into the bloodstream, allowing the clinician to rapidly achieve and fine-tune the desired level of sedation. IV sedation is especially useful for longer or more invasive procedures and for patients who require a deeper level of relaxation than oral medication or nitrous oxide can provide.
With IV techniques, the provider can adjust the medication in real time to maintain an appropriate depth of sedation. Careful monitoring of heart rate, oxygen levels, and blood pressure is standard practice, and the treatment team remains prepared to respond to any changes in the patient’s status. The oral surgeon’s training in anesthesia and airway management supports safe delivery of IV sedation in an outpatient setting.
Because IV sedation produces a stronger effect, additional precautions are necessary. Patients receive specific instructions about preoperative fasting and must arrange transportation home. The team discusses recovery expectations and provides clear guidance on post-procedure activity until the sedative’s effects have fully worn off.
In some cases, general anesthesia may be recommended for complete unconsciousness during complex or extensive procedures. When general anesthesia is used, it is administered and monitored according to established safety standards to protect the patient’s airway, breathing, and cardiovascular function throughout the case.
Whether a patient needs mild relaxation or deeper sedation, modern monitoring and experienced clinicians ensure that comfort does not come at the expense of safety. The combination of local anesthesia and appropriate sedative techniques allows effective pain control and a calm procedural experience.
To learn more about how sedation dentistry can make your oral surgery safer and more comfortable, please contact us for additional information and guidance. Our team is available to discuss options and help you prepare for a relaxed, well-managed visit.

Sedation dentistry offers patients with general anxiety or fears about a dental procedure the opportunity to have a more comfortable and stress-free experience. By utilizing safe and controlled sedation techniques, the patient is eased into a state of complete relaxation before the procedure. This approach eliminates discomfort, pain, and preoperative anxiety, and typically makes patients feel more at ease post-operatively, as they have little or no memory of the actual moment-to-moment procedure.
Local anesthesia involves an injection directly into or close to the area where a procedure is being performed. While it eliminates any sensation of pain in the targeted area, it does not affect your state of mind or level of anxiety. When a patient receives sedation, additional medications to ease anxiety and promote relaxation are employed in advance of local anesthesia. In this way, both the stress and discomfort associated with a procedure are eliminated. Sedation can be administered in a variety of forms based upon patient needs and the recommendations of the dentist or dental anesthesiologist.
Choosing the most appropriate method of sedation for a procedure depends on a variety of factors such as a patient's medical history and their level of anxiety. Dental sedation can come in the form of nitrous oxide sedation, oral conscious sedation, and IV sedation. Certain patients receiving comprehensive treatment or undergoing a complex surgical procedure may require general anesthesia in a hospital setting.
Nitrous oxide, or "laughing gas," is a mild sedative, which is inhaled through a small mask over the nose. A standard in dental sedation for decades, the effects of nitrous oxide are almost immediate and wear off quickly once your procedure is completed.
Oral sedation involves the prescription of an oral medication prior to your appointment. Taken at the recommended time before your visit, oral sedation allows you to feel fully relaxed by the time you're ready for your procedure. With oral sedation, it's necessary to plan on having an escort to and from your dentist's office.
IV Sedation is administered intravenously, or directly into a vein. It is typically indicated when a deeper state of sedation is required. Your dentist will provide you with specific instructions before your visit, and require that you have an escort for the trip home from your appointment.
Sedation dentistry uses medications to reduce anxiety and increase comfort for patients undergoing oral and maxillofacial procedures. Sedation can range from mild relaxation with nitrous oxide to deeper IV sedation or general anesthesia for more complex cases, and it is used in combination with local anesthetic to control pain at the surgical site. The primary goals are to keep patients calm, minimize movement, and allow the surgeon to work safely and efficiently.
At Pharos Implants and Oral Surgery we tailor sedation to each patient’s needs through careful assessment and monitoring, ensuring a calm, well-managed experience. The use of sedation often reduces memory of the procedure, which many patients find helpful in easing long-term anxiety about dental care. Safety and clear communication are emphasized so patients understand what to expect before, during, and after treatment.
Candidates for sedation include patients who experience significant dental anxiety, those undergoing lengthy or complex procedures, and people with a strong gag reflex or difficulty remaining still. Sedation can also be appropriate for patients with certain medical or developmental conditions that make cooperation challenging during treatment. The decision is individualized and based on medical history, procedure complexity, and patient preference.
During the preoperative evaluation the surgeon reviews current medications, prior anesthesia experiences, and any health conditions that could affect breathing or cardiovascular function. This review helps determine which level of sedation is both safe and effective. If deeper sedation is recommended, the team will discuss logistical needs such as fasting and arranging a responsible escort.
Common sedation options include nitrous oxide, oral sedation, intravenous (IV) sedation, and general anesthesia, each offering different depths of relaxation and control. Nitrous oxide is a mild inhaled sedative that works quickly and wears off rapidly, while oral sedatives are taken ahead of the appointment to produce predictable relaxation. IV sedation delivers medication directly into the bloodstream for fast onset and precise titration, and general anesthesia provides complete unconsciousness for extensive or highly invasive procedures.
Each method has advantages depending on procedure length, patient anxiety level, and medical history, and local anesthetic is typically used alongside sedation to ensure the surgical site is numb. The team will explain the expected level of awareness, how memory may be affected, and recovery expectations for the chosen method. Clear monitoring and airway management are part of standard protocols for all but the lightest forms of sedation.
Safety is maintained through thorough preoperative assessment, appropriate selection of sedation technique, and continuous monitoring of vital signs during the procedure. Standard monitoring typically includes heart rate, blood pressure, oxygen saturation and, when indicated, respiratory monitoring to ensure stable breathing and circulation. The clinical setting is equipped and the team is trained to respond to changes in patient status, with airway management skills and emergency equipment readily available.
Oral and maxillofacial surgeons receive specialized training in anesthesia and perioperative care, which supports safe sedation administration in an outpatient environment. Protocols such as preoperative fasting for deeper sedation, medication reconciliations, and documented consent reduce risk and enhance preparedness. Patients are given clear instructions about post-procedure activity and observation until they meet criteria for safe discharge.
The right sedation plan emerges from a comprehensive evaluation that includes medical history, current medications, prior anesthesia reactions, and the specific nature of the planned procedure. The surgeon assesses factors such as airway anatomy, cardiac or respiratory conditions, and potential drug interactions to select the safest, most effective option. Patient preferences and past experiences with dental care are also considered to ensure comfort and cooperation.
Preoperative discussions cover expected effects, recovery timelines, and any special instructions such as fasting or medication adjustments, so patients can make an informed decision. In some cases the surgeon, such as Dr. Joshua Munson, may recommend a particular level of sedation based on clinical judgment and training in anesthesia management. Consent and thorough communication are documented before proceeding to ensure shared understanding and safety.
Preparation steps vary with the level of sedation but commonly include following fasting guidelines, arranging a responsible adult to drive and accompany the patient home, and reviewing current medications with the surgical team. Patients should provide a complete medical history and disclose supplements, over-the-counter drugs, and any recreational substances to avoid adverse medication interactions. Clear directions about when to stop eating and drinking will be given for deeper sedation or general anesthesia.
On the day of the appointment patients should wear comfortable clothing and bring any required documentation or a list of medications. It is important to follow the team’s instructions about hygiene and removal of jewelry or contact lenses to support safe monitoring and airway care. If there are questions or concerns before the procedure, contacting the office ahead of time helps address issues and reduces day-of anxiety.
Recovery expectations depend on the sedation type; lighter methods like nitrous oxide allow most patients to resume normal activities quickly, while oral and IV sedatives may produce drowsiness for several hours. After deeper sedation or general anesthesia patients are monitored until vital signs are stable and protective reflexes have returned, and discharge instructions cover activity restrictions, eating and drinking, and medication management. A responsible adult should remain with patients until they are sufficiently alert and able to follow instructions safely.
Patients may experience temporary side effects such as grogginess, dry mouth, or mild nausea, which typically resolve within hours but should be discussed if persistent. The surgical team provides specific guidance on pain control, wound care, and signs that warrant prompt contact with the office. Follow-up appointments or phone check-ins are arranged as needed to ensure healing proceeds smoothly.
Sedation often improves procedural efficiency because a relaxed, cooperative patient reduces unexpected movement and allows the surgeon to work without interruption. For complex or multiple procedures performed in a single visit, deeper sedation can facilitate a more controlled operating environment and help the surgeon maintain precision. Many patients also report a more positive perioperative experience when anxiety is reduced, which can make follow-up care and recovery less stressful.
However, the primary focus remains on safety and appropriate technique rather than speed, and the chosen sedation method is matched to the clinical requirements of the case. The team balances procedural needs with patient health considerations to optimize outcomes and minimize risk. Clear communication about expectations helps align the patient’s goals with the clinical plan.
Yes, conditions such as obstructive sleep apnea, severe respiratory disease, major cardiac issues, liver or kidney impairment, and certain neurological disorders can influence which sedation techniques are safe. Many prescription and over-the-counter medications, as well as herbal supplements, may interact with sedatives or affect anesthesia metabolism, so a detailed medication review is essential. Smoking, alcohol use, and recreational drug use can also alter sedative effects and are important to disclose.
Knowing these factors allows the surgical team to modify dosages, select alternative medications, or recommend additional monitoring to enhance safety. In some cases consultation with a patient’s primary care physician or a medical specialist is arranged to coordinate care. The preoperative assessment is designed to identify and mitigate risks before any sedative is administered.
If you have questions about sedation or want to discuss options for an upcoming procedure, contact our office to schedule a consultation where your medical history and treatment needs can be reviewed. Our team will explain the available sedation methods, expected effects, and any preparatory steps so you can make an informed choice that aligns with your comfort level and safety. We encourage patients to bring a list of current medications and to share prior anesthesia experiences during the visit.
Pharos Implants and Oral Surgery strives to create a supportive environment where patients feel heard and well informed about their sedation plan. If deeper sedation is appropriate the staff will provide clear instructions about fasting, escort arrangements, and postoperative care to ensure a smooth, well-managed visit. Please call or use our online contact options to arrange a personalized evaluation and to address specific concerns before your procedure.

Our friendly and knowledgeable team is ready to help you schedule appointments, answer questions about procedures, and address any concerns. Whether by phone or our easy online contact form, we’re here to make your experience simple and convenient.
Take the first step toward restoring your smile and discover the difference personalized, expert care can make. Contact us today and let us help you achieve the confident, healthy smile you deserve.