
Request Appointment
Our Location
Monday
Closed
Tuesday
8:00 am - 5:00 pm
Wednesday
8:00 am - 5:00 pm
Thursday
8:00 am - 5:00 pm
Friday
8:00 am - 1:00 pm
Saturday
Closed
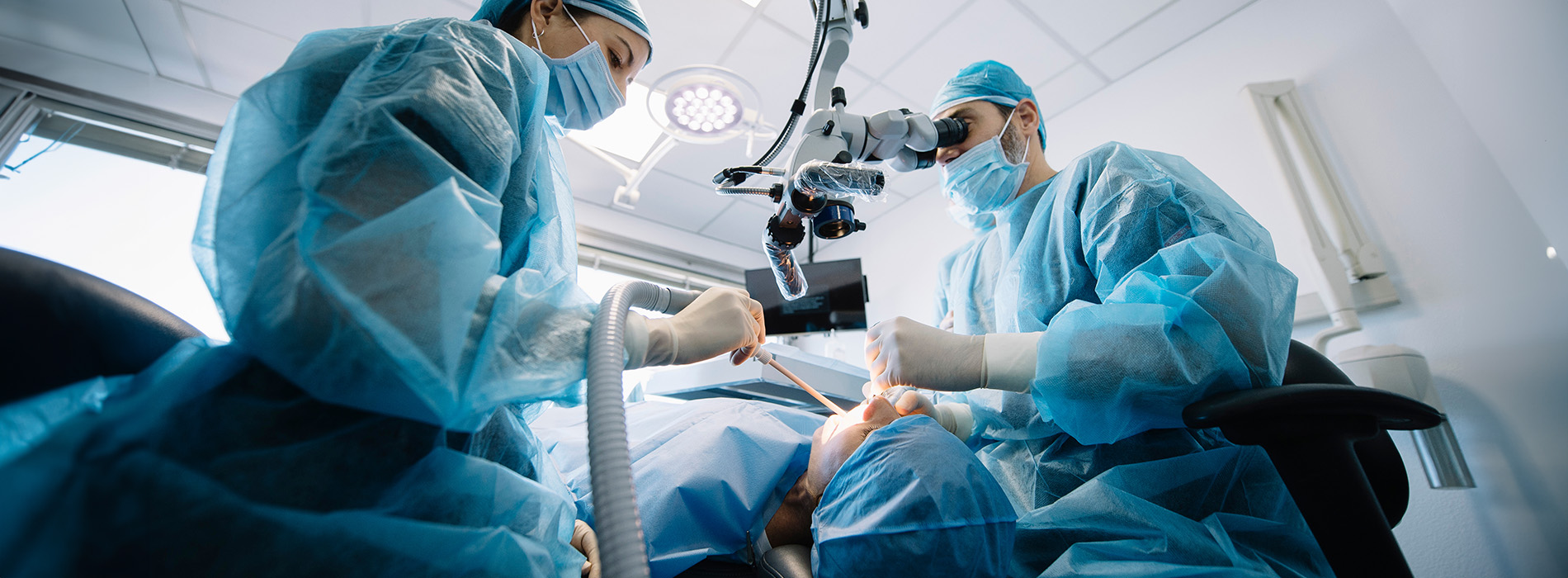
Oral surgery is a surgical specialty focused on diagnosing and treating a broad range of problems that affect the mouth, jaws, and facial structures. While many dental concerns are handled by general dentists, oral surgery addresses situations that require advanced training in anatomy, surgical technique, and anesthesia. The goal is to restore function, relieve pain, and support long-term oral health with procedures tailored to each patient’s needs.
Patients seek oral surgery for many reasons: removal of teeth that can’t be saved, repair of injury after trauma, correction of developmental or acquired jaw deformities, and management of conditions that threaten oral health. Some treatments are straightforward and brief, while others follow a staged approach to rebuild bone or soft tissue before definitive restoration. In every case, careful evaluation and planning guide the surgical approach.
Because oral surgery frequently touches both dental and medical concerns, it emphasizes safety and comfort. Surgeons use advanced imaging and diagnostic tools to form a clear picture of the problem and to plan treatment that balances effectiveness with recovery considerations. This focus on precision and patient well-being helps people regain function and confidence more predictably.
The spectrum of oral surgery procedures is wide. Routine surgical care includes extraction of erupted or impacted teeth, surgical root-end procedures (apicoectomies), and exposure of impacted teeth to aid orthodontic treatment. These procedures help address pain, infection, or alignment issues that conservative dentistry cannot resolve.
Reconstructive and preparatory procedures are also common. Bone grafts, sinus lifts, and ridge augmentation rebuild the jaw so it can support dental restorations like implants or well-fitting dentures. Pre-prosthetic surgery and tissue recontouring optimize the shape of bone and soft tissue to improve fit, function, and esthetics of future prosthetic work without prematurely committing to a specific restoration.
Oral surgeons also manage urgent and complex problems including facial trauma, infected teeth or spaces, and biopsies or removal of suspicious lesions. Treatments for obstructive sleep apnea and evaluation/treatment of temporomandibular joint (TMJ) disorders fall under the same umbrella when surgical options are appropriate. When a procedure requires coordination with your dentist, orthodontist, or medical specialists, the surgeon works as part of a care team to ensure continuity and clear communication.
A well-structured plan begins with a thorough clinical evaluation. During an initial consultation, the surgeon reviews your medical and dental history, performs an oral and facial exam, and discusses symptoms and goals. Understanding overall health is essential because it can influence surgical choices and anesthesia considerations.
Modern imaging plays a central role in planning. Panoramic X-rays, cone-beam computed tomography (CBCT), and intraoral photos allow the surgeon to visualize bone volume, tooth position, and relationships to vital structures such as nerves and the sinus. This level of detail helps minimize surprises during surgery and supports more predictable outcomes.
Treatment recommendations are tailored to the individual. The surgeon will explain available options, outline the expected course of the procedure, and discuss postoperative recovery. Emphasis is placed on informed decision-making so patients understand what to expect and can weigh benefits and limitations relative to their goals for function and appearance.
Comfort and safety are central concerns in oral surgery. Surgeons receive advanced training in anesthesia and sedation, allowing them to offer a range of options from local anesthesia to oral or IV sedation and, when appropriate, general anesthesia. The choice depends on the complexity of the procedure, patient health, and anxiety levels. Prioritizing monitoring and established protocols helps keep patients comfortable throughout treatment.
Recovery varies by procedure. Minimally invasive surgeries may involve a day or two of mild discomfort and simple home care, while more extensive reconstructions can require a longer healing period with staged follow-up visits. Patients receive clear instructions on wound care, medications, diet modifications, and activity restrictions to support safe healing. Follow-up appointments help ensure recovery is progressing as expected.
Predictable pain control, infection prevention, and stepwise rehabilitation are emphasized rather than promises of instant results. The surgical team coordinates with referring dentists and other specialists to align timing for restorative work—such as placing implants or fitting prostheses—so functional and cosmetic goals are met without compromising healing.
Many restorative solutions depend on having adequate bone and soft tissue support. Procedures like bone grafting, guided bone regeneration, and sinus augmentation restore or augment the jaw so it can safely support dental implants or provide the proper contours for dentures. These interventions are often planned well in advance of final restorations to allow the body time to integrate new graft material and rebuild a stable foundation.
Grafting techniques use a variety of materials and approaches selected for each case. Autogenous grafts (from the patient), processed bone products, and synthetic alternatives each have roles depending on availability and clinical goals. The choice reflects a balance of biology, patient preference, and the long-term needs of the restoration.
Soft tissue management is equally important. Procedures to reposition or reshape gum tissue, or to perform pre-prosthetic contouring, create the ideal environment for oral function and esthetics. Thoughtful sequencing of bone and soft tissue procedures with implant placement or prosthetic fabrication improves the likelihood of durable, natural-looking outcomes.
At Pharos Implants and Oral Surgery, our approach is rooted in careful diagnosis, clear communication, and surgical precision. Whether you need a single tooth extraction, complex reconstruction, or urgent trauma care, our team is prepared to evaluate your situation and recommend a treatment path that prioritizes safety and long-term oral health.
To learn more about oral surgery options and what to expect for your care, contact us for additional information. Our team can help you understand the next steps and schedule an evaluation to determine the right plan for your needs.

Oral surgery is a surgical specialty that diagnoses and treats problems affecting the mouth, jaws and related facial structures. It covers issues that require advanced training in anatomy, surgical technique and anesthesia beyond what general dentistry typically manages. The goal of these interventions is to restore function, relieve pain and support long-term oral health through tailored procedures.
Common reasons patients seek oral surgery include teeth that cannot be saved, impacted or problematic wisdom teeth, facial trauma, jaw deformities and suspicious oral lesions. Oral surgeons also perform preparatory and reconstructive work such as bone grafting and soft tissue contouring before restorative treatment. Because many cases intersect dental and medical concerns, care emphasizes safety, precise planning and coordinated communication with referring providers.
The range of oral surgery procedures spans simple to complex interventions performed in the office or an ambulatory setting. Routine procedures include extractions of erupted or impacted teeth, apicoectomies to treat persistent root infections and surgical exposure of impacted teeth to assist orthodontic movement. Reconstructive and preparatory procedures such as bone grafts, ridge augmentation, sinus lifts and pre-prosthetic contouring help create stable foundations for implants and dentures.
Oral surgeons also manage facial trauma, remove suspicious lesions or perform biopsies, and provide surgical options for select temporomandibular joint and sleep apnea cases. Implant placement and staged implant restoration planning are frequent services when replacing missing teeth. Each procedure is chosen and sequenced based on clinical need, biologic considerations and the patient's treatment goals.
Care begins with a comprehensive evaluation that includes a review of medical and dental history, a clinical exam and a discussion of symptoms and expectations. Understanding overall health, medications and prior treatments is critical because these factors influence surgical choices and anesthesia planning. The surgeon will explain options and help patients weigh benefits, risks and expected recovery to support informed decision-making.
Advanced imaging is central to precise planning and predictable outcomes. Panoramic X-rays, cone-beam computed tomography (CBCT) and intraoral photography reveal bone volume, tooth position and relationships to vital structures like nerves and the sinus. This detailed visualization minimizes intraoperative surprises and guides decisions about grafting, implant size and implant trajectory, supporting safer, more effective procedures.
Oral surgeons are trained to deliver a spectrum of anesthesia and sedation options to match the procedure and patient needs. Options commonly range from local anesthesia for simple procedures to oral or intravenous sedation and general anesthesia for more complex surgeries or for patients with high anxiety. The choice is based on the extent of surgery, the patient's medical history and their comfort preferences.
Regardless of the modality, emphasis is placed on monitoring and safety throughout the procedure. Patients are evaluated beforehand to identify medical conditions or medications that could affect anesthesia, and clear preoperative instructions are provided when sedation or general anesthesia is planned. The surgical team follows established protocols for vital signs monitoring and recovery to help ensure a safe experience.
Preparation begins with a thorough preoperative review of your health history, medications and any allergies so the surgeon can tailor anesthesia and perioperative care. If sedation or general anesthesia is planned, patients will receive fasting instructions and guidance about which medications to take or temporarily hold before surgery. Arranging a responsible adult to drive you home and help during the initial recovery period is important whenever sedation is used.
Practical steps such as filling prescriptions ahead of time, wearing comfortable clothing and planning for a soft-food diet after the procedure can simplify recovery. Bring a list of current medications and any recent imaging or dental records if available, and communicate chronic health issues such as diabetes or bleeding disorders. Clear questions for the surgeon about what to expect on the day of surgery help reduce anxiety and improve readiness.
Recovery varies by procedure but generally follows predictable stages of swelling, gradual reduction in discomfort and progressive return to normal function. In the first 24 to 72 hours patients commonly experience some swelling and mild to moderate pain controlled with prescribed or recommended medications, ice application and rest. Soft foods, careful oral hygiene per instructions and avoiding strenuous activity help support uncomplicated healing.
Follow-up visits allow the surgeon to monitor healing, remove sutures if needed and coordinate timing for additional restorative steps such as implant placement or prosthetic work. Patients should watch for signs of complications such as uncontrolled bleeding, increasing pain, fever or persistent numbness and contact the office promptly if these occur. For questions about specific recovery expectations and when to resume normal activities, the office staff at Pharos Implants and Oral Surgery can provide guidance tailored to your procedure.
Bone grafting and sinus augmentation rebuild lost bone volume so dental implants have a stable, biologic foundation. Grafts may use the patient's own bone, processed donor bone or synthetic materials selected based on the clinical situation and the volume needed. Over time the graft integrates with native bone, creating sufficient height and width to support implants and help ensure long-term success.
A sinus lift raises the floor of the maxillary sinus to allow placement of implants in the upper back jaw where bone height is inadequate. These procedures are often staged so grafting heals before implants are loaded, which improves predictability in challenging sites. Careful planning with three-dimensional imaging helps determine the optimal grafting approach and timing relative to implant placement.
Oral surgeons are trained to manage a wide range of urgent and complex problems involving facial trauma, tooth avulsion, jaw fractures and soft tissue injuries. Prompt evaluation focuses on stabilizing the patient, addressing airway or bleeding concerns and planning definitive surgical repair of fractures or damaged teeth and tissues. Early intervention preserves function and minimizes long-term complications when possible.
Severe odontogenic infections or deep space infections that threaten surrounding structures may also require surgical drainage and targeted antibiotic therapy. When infection does not respond to conservative measures or when it involves spreading cellulitis, surgical management in conjunction with medical oversight is often necessary. The surgeon collaborates closely with medical colleagues for cases requiring hospitalization or advanced airway management.
Oral surgeons frequently work as part of a multidisciplinary team that includes general dentists, prosthodontists, orthodontists and medical specialists. Coordination ensures that surgical timing aligns with restorative plans, orthodontic movement or medical treatments and that each provider understands the sequence of care. Clear communication and shared records help reduce delays and improve outcomes for complex cases.
For conditions such as TMJ disorders, obstructive sleep apnea or oncologic concerns, the surgeon participates in joint planning with relevant specialists to balance surgical, functional and medical priorities. This team-based approach allows individualized treatment plans that address both immediate surgical needs and long-term oral health goals for the patient.
Your general dentist will often manage routine dental care but may refer you to an oral surgeon for conditions that require advanced surgical or anesthesia expertise. Appropriate reasons for referral include complex extractions, impacted wisdom teeth, significant bone loss requiring grafting, facial trauma, suspicious oral lesions needing biopsy and cases where deeper sedation or general anesthesia is recommended. Referral also makes sense when multidisciplinary coordination is needed for dental implants or jaw deformity correction.
Seeking an evaluation from a specialist can provide clarity on treatment options and sequencing, and the surgeon can work with your dentist to implement a coordinated plan. If you are considering surgical treatment, the office of Pharos Implants and Oral Surgery can perform a focused assessment and explain why a surgical referral is recommended or whether conservative management remains appropriate.

Our friendly and knowledgeable team is ready to help you schedule appointments, answer questions about procedures, and address any concerns. Whether by phone or our easy online contact form, we’re here to make your experience simple and convenient.
Take the first step toward restoring your smile and discover the difference personalized, expert care can make. Contact us today and let us help you achieve the confident, healthy smile you deserve.