Request Appointment
Our Location
Monday
Closed
Tuesday
8:00 am - 5:00 pm
Wednesday
8:00 am - 5:00 pm
Thursday
8:00 am - 5:00 pm
Friday
8:00 am - 1:00 pm
Saturday
Closed

Oral and facial injuries demand prompt, experienced care to protect both function and appearance. When trauma affects the mouth, jaw, or face, the right surgical team can reduce pain, lower the risk of long-term complications, and preserve the structures that support eating, speaking, and smiling. Treatment ranges from quick on-site stabilization to staged reconstructive approaches that restore alignment and comfort over time.
At Pharos Implants and Oral Surgery, our approach emphasizes clear communication, careful assessment, and tailored treatment plans. We work with referring dentists, endodontists, and medical specialists when needed to coordinate care, monitor healing, and transition patients smoothly from emergency management to long-term restoration.
The first minutes and hours after an oral or facial injury are critical. Our team focuses on rapid but thorough evaluation: checking the airway and breathing first, then assessing bleeding, swelling, and the stability of teeth and facial bones. Stabilization often includes controlling hemorrhage, protecting exposed tissues, and addressing any threats to airway safety before proceeding to more detailed imaging and planning.
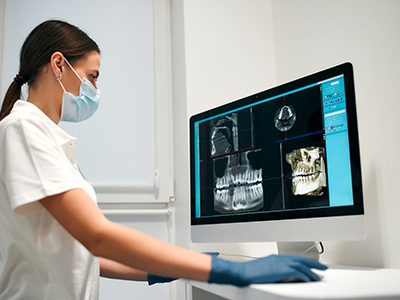
Imaging—typically panoramic radiographs, cone beam CT, or targeted dental films—helps reveal fractures, displaced teeth, and sinus or orbital involvement that aren’t obvious on visual exam alone. This diagnostic information guides whether immediate surgery is needed or whether a temporary, conservative approach is appropriate while swelling decreases and tissues are reassessed.
When injuries require urgent treatment, our priorities are preserving viable tooth structure, minimizing soft tissue damage, and restoring anatomical relationships so healing can occur with the best possible functional and cosmetic outcome. Patients are reassured with a clear plan that outlines immediate steps, expected follow-up, and coordination with other dental or medical providers.
A chip or crack in a tooth can be a simple cosmetic problem or the start of a more complex situation that compromises the tooth’s long-term health. Minor enamel chips are often repaired with a bonded restoration, while deeper fractures that extend into dentin or the pulp may require endodontic treatment and full coverage restorations to prevent infection and restore strength.
When a fracture involves the root or splits a tooth vertically, the outlook changes. Some fractures can be managed with careful stabilization and restorative work, but others—particularly those that extend below the gumline—may be unrestorable and require extraction. The surgeon’s assessment includes evaluating the extent of the crack, the tooth’s periodontal support, and the patient’s overall dental plan.
For compromised teeth that are lost or must be removed, modern reconstructive options such as bone grafting and dental implants can restore chewing function and appearance while preserving adjacent teeth. Timing and sequencing of these treatments are individualized based on the injury, healing progress, and collaboration with the patient’s restorative dentist.
Dentoalveolar trauma involves the teeth and the alveolar bone that holds them. These injuries range from subluxations—teeth that are loosened but stay in place—to luxations where teeth are displaced, and avulsions where a tooth is completely knocked out. Rapid attention improves the chances of saving displaced or avulsed teeth and preserving the surrounding bone.
Treatment often begins with careful repositioning and stabilization using splints or other fixation methods to allow reattachment and healing. In cases where a fragment of alveolar bone is involved, the surgeon repairs and stabilizes the bone to reestablish proper alignment and support for the teeth. Antibiotics and tetanus status are considered as appropriate for traumatic wounds.
Follow-up care is essential: teeth that have undergone traumatic displacement need periodic monitoring for vitality, root resorption, or changes in attachment. The oral and maxillofacial surgeon works closely with general dentists and endodontists to determine when additional intervention—such as root canal therapy or restorative procedures—is needed to secure long-term tooth viability.
Cuts and lacerations of the lips, cheeks, tongue, and gums are common in facial trauma. Soft tissue repair is more than closing a wound; it’s about aligning layers precisely to restore sensation, mobility, and a natural appearance. That requires careful attention to tissue margins, thoughtful selection of suture material, and an eye for aesthetic outcome as well as function.
When a wound involves the oral mucosa or extends into deeper tissues, the surgeon assesses for foreign bodies, nerve injury, and damage to salivary ducts. Repair may include layered closure, debridement of nonviable tissue, and measures to reduce scarring and preserve oral competence. Early, appropriate repair reduces the risk of infection and improves long-term comfort and appearance.
In complex cases—where significant tissue loss or contaminated wounds are present—staged reconstruction may be necessary. This can involve local tissue rearrangement, grafting, or collaboration with plastic surgery colleagues. Regardless of the approach, the goal is to restore natural form and function while minimizing visible scarring and sensory changes.
Fractures of the jaw, cheekbone, orbital rim, and nasal bones can affect chewing, vision, breathing, and facial symmetry. Treatment decisions hinge on the location and severity of the fracture, the patient’s overall health, and the timing of intervention. Some fractures can be managed non-surgically with a soft diet and close monitoring, while others require precise surgical repair.
Surgical repair typically aims to realign bone segments, stabilize them with plates and screws when indicated, and reestablish the normal facial contours. For mandibular fractures, rigid fixation allows early return to function; orbital fractures may require reconstruction to prevent double vision or enophthalmos; and midface injuries are managed to restore occlusion and cheek projection.
Recovery includes pain control, infection prevention, and stepwise return to normal activity. The surgeon evaluates healing through clinical exams and follow-up imaging, adjusting care to address complications such as malocclusion, persistent numbness, or hardware concerns. When needed, secondary procedures can refine form and function after initial healing.
Oral and facial trauma can be unsettling, but timely, expert care reduces risks and speeds recovery. If you or someone you care for has sustained an injury to the teeth, mouth, or face, prompt evaluation is important to preserve function and appearance. Pharos Implants and Oral Surgery is committed to thorough assessment and coordinated treatment—please contact us for more information about our approach to trauma care and to arrange an evaluation.

Oral and facial trauma refers to injuries that affect the mouth, teeth, jaws, and surrounding facial tissues, including soft tissue lacerations and fractures of the facial bones. These injuries commonly result from falls, sports incidents, motor vehicle collisions, interpersonal violence, and occupational accidents. Because structures in the face support breathing, chewing, speech and appearance, prompt evaluation is important to protect both function and long-term form.
Trauma cases range from minor chips and soft tissue cuts to complex fractures and avulsed teeth that require multidisciplinary care. Initial assessment focuses on airway safety, bleeding control and the stability of teeth and bones, while imaging and specialist consultation guide definitive treatment. Timely, well-coordinated care reduces the risk of complications such as infection, malocclusion and chronic pain.
Begin by ensuring the scene is safe and then check the injured person’s airway, breathing and level of consciousness; call emergency services if there is any concern about breathing or major bleeding. Apply gentle pressure with a clean cloth to control bleeding and keep the head elevated to reduce swelling when possible, taking care not to move unstable facial bones or displaced teeth. If a tooth has been knocked out, handle it by the crown only and, if feasible, place it in milk or sterile saline to help preserve it for possible reimplantation.
Avoid trying to reinsert a tooth if the patient is unconscious or if you are unsure how to do so safely; instead, seek professional care immediately. Prompt arrival at an emergency department or an oral and maxillofacial surgery practice allows for airway assessment, imaging and stabilization. The surgical team will address immediate threats, plan definitive repair and coordinate follow-up with dental and medical colleagues as needed.
Evaluation of a fractured tooth begins with a clinical exam and imaging, such as periapical films or cone beam CT, to determine the extent of the break and whether the pulp or root is involved. The clinician assesses symptoms, tooth mobility, periodontal support and any associated injuries to surrounding bone or soft tissue. Distinguishing between superficial enamel chips, deeper crown fractures and root or vertical fractures is essential because each has different implications for prognosis and treatment.
Treatment ranges from conservative bonding or a crown for enamel and dentin injuries to root canal therapy and full-coverage restoration when the pulp is affected. Teeth with vertical root fractures or those split below the gumline may be unrestorable and require extraction, after which options such as bone grafting and implant placement can be considered. The oral surgeon works with the patient’s restorative dentist to sequence care and optimize functional and aesthetic outcomes.
The likelihood of saving an avulsed tooth depends strongly on the time it spends out of the socket and how it is stored, with immediate reimplantation offering the best chance of success. A tooth kept moist in milk or saline and brought promptly to a clinician has a higher probability of reattachment than one that is dry for an extended period. The stage of root development, the condition of the socket and any associated alveolar bone injury also influence prognosis.
When reimplantation is performed, the tooth is typically stabilized with a splint and the patient is monitored closely for infection, root resorption or loss of vitality. Root canal therapy is often required for mature teeth after reimplantation, and long-term follow-up is necessary to assess healing. If a tooth cannot be saved, restorative options such as implants or fixed prosthetics are planned in coordination with the patient’s overall dental care.
Bone grafting is considered when trauma results in significant loss of alveolar bone or when a tooth is lost and the bony ridge needs rebuilding to support future restoration. Grafting can preserve or restore ridge volume, provide a stable foundation for implants and improve aesthetic outcomes in the long term. The choice and timing of grafting—immediate at the time of extraction or delayed after soft tissue healing—depend on socket condition, presence of infection and the quality of remaining bone.
Dental implants are typically planned after adequate bone healing and imaging confirmation, often several months after grafting when necessary. Precise implant placement requires three‑dimensional assessment and coordination with the restorative dentist to restore function and appearance. Your surgeon will discuss the sequence of grafting, implant placement and provisional restorations to achieve predictable results tailored to your recovery.
Repair of facial and oral soft tissue injuries focuses on restoring function and achieving the best possible cosmetic result by aligning tissues accurately and using appropriate suture materials. The surgeon inspects wounds for foreign bodies, assesses nerve and salivary duct involvement, and debrides any nonviable tissue before closure. Layered closure is frequently used in deeper wounds to reapproximate muscle and mucosal or skin layers separately, which helps preserve mobility and reduces visible scarring.
Intraoral wounds are usually closed with absorbable sutures, while skin lacerations may require fine nonabsorbable sutures removed after appropriate healing time. Prophylactic antibiotics and tetanus updates are considered when contamination is present or the wound is complex. For extensive tissue loss or contaminated injuries, staged reconstruction using local flaps or grafts may be planned to restore oral competence and facial contours.
Common facial fractures include mandibular (jaw) fractures, zygomaticomaxillary complex fractures (cheekbone), orbital floor and rim fractures, nasal fractures and midface (Le Fort) fractures. Each type can affect critical functions such as chewing, breathing and vision, and the severity of displacement and involvement of adjacent structures determines treatment urgency. Detailed imaging, often with cone beam or CT scans, helps define fracture patterns and guides surgical planning.
Treatment options range from conservative management with soft diet and observation to open reduction and internal fixation with plates and screws for displaced fractures. Mandibular fractures often benefit from rigid fixation to restore occlusion and allow early function, while orbital fractures may require reconstruction to prevent double vision or enophthalmos. Postoperative care includes pain management, infection prevention and monitoring for complications such as malocclusion, numbness or hardware issues.
Effective trauma care frequently involves a team approach that may include the patient’s general dentist, endodontist, prosthodontist, plastic surgeon, otolaryngologist, ophthalmologist and emergency medicine clinicians. The oral and maxillofacial surgeon communicates imaging findings, treatment plans and timelines to referring providers to ensure continuity from emergency stabilization through definitive restoration. Collaboration is particularly important when planning implants, complex reconstructions or when multiple systems are affected.
This coordinated approach helps sequence care so that acute needs are addressed promptly while long-term functional and aesthetic goals are integrated into the treatment plan. Shared records, joint consultations and staged procedures allow the team to minimize complications and align surgical and restorative steps for optimal patient outcomes. Patients benefit from a single point of surgical leadership that organizes multidisciplinary care around their specific needs.
Recovery after oral or facial trauma typically involves an initial period of swelling, bruising and controlled discomfort that decreases over days to weeks with appropriate care and medication. Patients are often advised to follow a modified diet, avoid strenuous activity for a prescribed period and maintain careful oral hygiene to support healing. The surgeon provides instructions for wound care, pain control and signs of complications that warrant prompt re-evaluation.
Follow-up visits include clinical checks and repeat imaging as needed to confirm bone healing, tooth vitality and soft tissue recovery, with splint removal or suture removal scheduled according to the procedure. Some patients require additional procedures—such as secondary refinements, root canal therapy or restorative work—once initial healing is complete. Long-term monitoring helps detect late complications like root resorption, infection or sensory changes so they can be managed proactively.
Seek immediate evaluation for signs of airway compromise, uncontrolled bleeding, severe facial swelling that limits breathing or eye closure, sudden vision changes, a displaced or avulsed tooth and injuries that cause deformity or inability to open or close the mouth. These symptoms may indicate life‑threatening problems or injuries that require urgent stabilization and imaging. Rapid assessment helps protect airway and vision and improves the chance of preserving teeth and function.
Pharos Implants and Oral Surgery offers urgent evaluation for traumatic injuries and coordinates care with local emergency services and medical specialists when needed; call the office at (704) 464-2888 to arrange prompt assessment or to determine the next appropriate step. When in doubt about airway safety or severe bleeding, proceed to the nearest emergency department or call emergency services immediately for immediate intervention.

Our friendly and knowledgeable team is ready to help you schedule appointments, answer questions about procedures, and address any concerns. Whether by phone or our easy online contact form, we’re here to make your experience simple and convenient.
Take the first step toward restoring your smile and discover the difference personalized, expert care can make. Contact us today and let us help you achieve the confident, healthy smile you deserve.