Request Appointment
Our Location
Monday
Closed
Tuesday
8:00 am - 5:00 pm
Wednesday
8:00 am - 5:00 pm
Thursday
8:00 am - 5:00 pm
Friday
8:00 am - 1:00 pm
Saturday
Closed

Healthy jawbone is the foundation for chewing, clear speech, and a natural facial profile. When teeth are lost or periodontal disease progresses, the underlying bone no longer receives the mechanical stimulation that keeps it strong. Over time this can lead to a reduction in both height and width of the ridge that supports teeth and soft tissues — changes that affect how dentures fit, how implants perform, and even how the lower third of the face appears.
Bone loss is more than a structural concern; it affects function and long-term treatment options. Without adequate bone volume, restorative choices such as dental implants may be limited or require additional preparatory procedures. Early assessment and timely intervention give patients more predictable outcomes and prevent the need for more extensive reconstruction later on.
This is why bone grafting is considered a proactive, restorative step in many treatment plans. By rebuilding lost bone, we aim to preserve facial contours, restore a stable foundation for replacement teeth, and protect adjacent structures so future dental care is both safer and more effective.
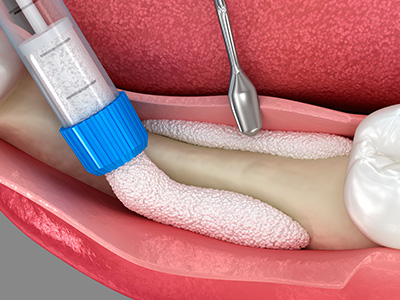
Bone grafts act as a scaffold and a biological stimulus. When graft material is placed into a deficient area, it provides a structure where native bone-forming cells can migrate and gradually replace the graft with the patient’s own bone. Depending on the material used, the graft may simply guide new tissue formation or actively encourage the body’s regenerative processes.
Materials for grafting fall into a few broad categories: the patient’s own bone (autograft), carefully screened donor bone (allograft), animal-derived materials (xenograft), and synthetic, biocompatible substitutes (alloplasts). Each option has advantages related to handling, availability, and how it integrates with existing bone. Your surgeon will recommend the approach best suited to your anatomy and treatment goals.
A successful graft restores volume and density, which improves the stability of implants and the fit of prosthetics. In many cases, grafting also helps reestablish the natural contours of the jaw so that prosthetic teeth and soft tissues look and feel more lifelike.
Grafting can be performed at different times depending on clinical needs. Socket preservation — placing graft material at the time of tooth extraction — is used to limit bone shrinkage immediately after removal. This preserves the ridge shape and often simplifies later implant placement. Alternatively, grafting can be done as a separate procedure once the area has healed and a deficiency is clearly defined.
Other common techniques address specific problems: ridge augmentation rebuilds a flattened or sunken ridge to support future restorations, while block grafts use larger pieces of bone to reconstruct significant defects. The choice between a softer particulate graft and a block or structural graft depends on how much three-dimensional support is required for the planned restoration.
Each case follows a clear treatment pathway: assessment and imaging to define the defect, selection of graft material and technique, surgical placement under local or IV sedation as appropriate, and a healing period during which the graft integrates with native bone. Close follow-up ensures the graft is maturing as expected before final restorative steps are taken.
When the upper back jaw has insufficient height for implants because of the nearby sinus cavity, a sinus lift (sinus augmentation) can create the necessary bone volume. During this procedure the sinus membrane is gently elevated and graft material is placed beneath it to build vertical height. Over the subsequent months this graft becomes transformed into functional bone that can reliably support implants.
Aesthetic ridge augmentation addresses contour defects that affect the appearance and function of a smile. These procedures focus on recreating natural ridge form so that fixed bridges or implant restorations sit in harmony with the lips and cheeks. In some situations, combining ridge augmentation with soft-tissue management produces the most natural-looking results.
Both sinus lifts and ridge augmentations are planned using three-dimensional imaging and careful anatomical assessment. This planning minimizes surprises during surgery and helps tailor the procedure to each patient’s unique needs and long-term restorative goals.
After a graft is placed, protecting it from movement, infection, and soft-tissue pressure is essential to successful integration. Surgeons commonly use barrier membranes to cover the grafted area — these membranes guide tissue regeneration by preventing faster-growing soft tissues from invading the graft site, allowing bone-forming cells the time and space they need to mature.
In some cases, biologically active agents such as platelet-rich fibrin or growth factors are applied to support healing and encourage faster, more complete bone formation. These adjuncts can enhance the body’s natural regenerative response without changing the overall surgical approach.
Recovery timelines vary: many grafts require several months to integrate fully before implants are placed. During this period, patients receive clear postoperative instructions on oral hygiene, activity restrictions, and appointments for monitoring. Certain factors — such as smoking or poorly controlled systemic conditions — can slow healing, so candid preoperative counseling helps set realistic expectations and optimize outcomes.
Bone grafting is a foundational technique for preserving function, restoring form, and enabling long-term dental restorations. Whether used immediately after extraction, to prepare the jaw for implants, or to correct contour defects, grafting gives clinicians the ability to rebuild bone in a controlled, predictable way.
If you’re considering tooth replacement or have experienced bone loss from disease or trauma, a surgical evaluation can clarify whether grafting is appropriate for your situation. The team at Pharos Implants and Oral Surgery offers experienced assessment and tailored treatment plans designed to restore both function and appearance.
Please contact us for more information or to schedule a consultation — we’re happy to explain your options and help you determine the best path forward for your oral health.

A bone graft is a surgical procedure that restores lost jawbone by placing graft material where bone volume is deficient. The graft acts as a scaffold that encourages the body's own bone-forming cells to migrate into the area and gradually replace the material with living bone. Restored bone volume improves the foundation for dental implants and supports surrounding teeth and soft tissues for better long-term function.
Bone grafting can be used proactively after extractions to preserve the ridge or later to rebuild areas that have resorbed from disease, trauma, or long-term tooth loss. By recreating the natural contours of the jaw, grafts also help prosthetics, such as implant crowns and bridges, look and fit more naturally. Proper planning and imaging guide the technique and timing to produce predictable outcomes.
Clinicians select graft materials from several categories including autografts (the patient’s own bone), allografts (carefully screened donor bone), xenografts (processed animal-derived materials), and alloplasts (synthetic biocompatible substitutes). Each material has different handling characteristics and biological behavior—autografts are often considered highly osteogenic while other options provide excellent scaffolding and avoid additional donor-site surgery. The choice depends on defect size, three-dimensional needs, and the overall treatment plan.
In addition to the primary graft material, surgeons frequently use barrier membranes to protect the graft and encourage bone regeneration by preventing soft-tissue ingrowth. Biologic adjuncts such as platelet-rich fibrin or growth factors may be applied to accelerate healing and support tissue integration in selected cases. Your surgeon will explain the advantages and trade-offs for the materials recommended for your situation.
Healing times vary with the graft type, location, and patient factors, but many grafts require several months for reliable integration before implant placement. Smaller socket-preservation grafts may be ready for implant planning in three to four months, while more extensive ridge augmentations or block grafts often need four to six months or longer to achieve adequate volume and density. Regular follow-up and imaging are used to confirm maturation before proceeding with definitive restoration.
Patient health influences healing speed; factors such as smoking, uncontrolled diabetes, or certain medications can slow bone formation and extend the timeline. During the healing period, clinicians advise protective measures to limit graft disturbance and infection risk while optimizing conditions for bone growth. Once imaging shows sufficient bone, the implant can be placed with greater confidence in long-term stability.
A sinus lift, or sinus augmentation, is a procedure to increase bone height in the upper back jaw when the sinus cavity has expanded and left insufficient bone for implants. The surgeon gently elevates the sinus membrane and places graft material beneath it to create vertical height that can support implants. This technique is commonly used when posterior maxillary bone loss or anatomical variations would otherwise limit implant options.
Sinus lifts are planned with three-dimensional imaging to evaluate sinus anatomy and avoid complications. Depending on the case, a simultaneous implant placement may be possible, or the graft may be allowed to heal before implants are placed. Careful postoperative instructions and monitoring help ensure predictable bone formation beneath the sinus membrane.
Ridge augmentation rebuilds a flattened or sunken alveolar ridge to recreate natural contours that support teeth and soft tissues. By restoring three-dimensional volume, the procedure improves the emergence profile and alignment of prosthetic teeth, which contributes to a more natural and balanced smile. When combined with appropriate soft-tissue management, ridge augmentation can significantly enhance both function and esthetics.
Techniques range from particulate grafting to block grafts depending on how much structural support is required for the planned restoration. The surgical approach is individualized to the defect and long-term prosthetic goals, with imaging used to guide the optimal graft placement. Healing and maturation are monitored before final restorative steps to ensure a stable foundation for implants or bridges.
Bone graft procedures are performed under local anesthesia with the option of conscious sedation or general anesthesia for greater comfort during more complex cases. During surgery the graft material is positioned to fill the defect and often covered with a membrane or sutured soft tissue to protect the site while healing begins. Most patients experience some swelling, mild to moderate discomfort, and temporary changes in chewing or speech that resolve over several days to weeks.
Postoperative instructions typically include guidance on oral hygiene, diet modifications, activity restrictions, and medications to manage pain and reduce infection risk. Follow-up appointments allow the surgical team to assess healing, remove sutures if needed, and confirm that the graft is integrating as expected. Promptly reporting unusual symptoms such as severe pain, persistent swelling, or fever helps address complications early.
Like all surgical procedures, bone grafting carries risks that include infection, wound dehiscence (opening), graft failure or resorption, and transient sensory changes when nerves are near the surgical site. Careful case selection, aseptic technique, and adherence to postoperative instructions minimize these risks and improve the likelihood of successful integration. In sinus lifts, additional considerations include sinus membrane perforation, which is managed during surgery to prevent long-term problems.
Systemic factors such as poor glycemic control, smoking, and certain medications can increase complication rates or delay healing, so candid preoperative evaluation is important. Your surgeon will discuss specific risks based on the planned procedure and anatomy and outline measures taken to reduce complications. Close follow-up and timely intervention if problems arise support the best possible outcome.
Good candidates are patients who have jawbone deficiencies that limit their ability to receive dental implants or that compromise the fit and appearance of prosthetics. Candidates generally should be in overall good health, with any systemic conditions such as diabetes well managed and a commitment to following postoperative instructions. Tobacco users are counseled about the negative impact of smoking on healing and encouraged to quit before and after surgery to improve success rates.
A thorough evaluation including clinical examination and three-dimensional imaging determines whether grafting is appropriate and which technique will best meet restorative goals. The surgeon will review medical history, current medications, and oral habits to ensure safe care and realistic expectations. Consultation with Dr. Joshua Munson or a member of the surgical team helps define a personalized treatment plan based on anatomy and long-term objectives.
Preparation includes reviewing your medical history, discontinuing or adjusting certain medications when advised by your surgeon and physician, and arranging transportation if sedation or general anesthesia is used. You should follow preoperative instructions regarding fasting, oral hygiene, and any antimicrobial rinses that reduce the risk of infection. Discuss tobacco use with your provider and make plans to stop or reduce smoking to enhance healing.
After surgery, avoid vigorous rinsing, spitting, using straws, or applying pressure to the graft site for the period recommended by your surgeon, as these actions can dislodge graft material or interfere with clot formation. Maintain gentle oral hygiene, follow dietary guidelines, and attend scheduled follow-up visits so the team can monitor integration and address concerns. Adhering to these measures helps protect the graft and supports predictable bone regeneration.
To begin, request an evaluation with the office of Pharos Implants and Oral Surgery so the surgical team can review your history and discuss treatment goals. Bring a list of current medications, any recent imaging or dental records you have, and a summary of medical conditions or allergies to help the surgeon plan a safe, effective approach. If you have existing dental radiographs or records from another provider, bringing them can streamline assessment and reduce the need for immediate additional imaging.
During the consultation you will receive a clinical exam and, when appropriate, three-dimensional imaging to define bone defects and guide recommendations. The surgeon will outline options, the proposed sequence of care, and the expected timeline for healing and restoration. This visit is an opportunity to ask specific questions about the procedure, anesthesia options, and postoperative care so you can make an informed decision about your treatment.

Our friendly and knowledgeable team is ready to help you schedule appointments, answer questions about procedures, and address any concerns. Whether by phone or our easy online contact form, we’re here to make your experience simple and convenient.
Take the first step toward restoring your smile and discover the difference personalized, expert care can make. Contact us today and let us help you achieve the confident, healthy smile you deserve.